Occlusion: What’s Behind a Bite?
According to the American Association of Orthodontists, occlusion is the relationship between your upper (maxillary) and lower (mandibular) teeth as they come into functional contact, such as when you bite, chew or close your jaws together. The way the occlusal (chewing) surfaces of any of your teeth come together affects the other teeth, in addition to your gums, your neck and head, the muscles of the jaw, the jaw joint and your oral health.
When your dentist examines your occlusion, he or she is looking at how chewing forces, or those forces that occur when your teeth come together, could cause a breakdown of the teeth, gums, muscles and joints. Force is also exerted on your teeth when they come together during clenching or grinding. Your dentist will assess what might be done, if necessary, to prevent or correct any problems associated with chewing force.
Evaluating Your Occlusion
There are a number of common signs that are indicative of malocclusion. People who experience these signs are advised to talk to their dentist about an occlusal evaluation. Signs that there might be a problem with your occlusion include:
- Excessive tooth wear
- Tooth breakage
- Tooth loss
- Previous root canals
- Tooth sensitivity
- Head and neck muscle pain
- Headaches
- Jaw joint pain
- Joint noises
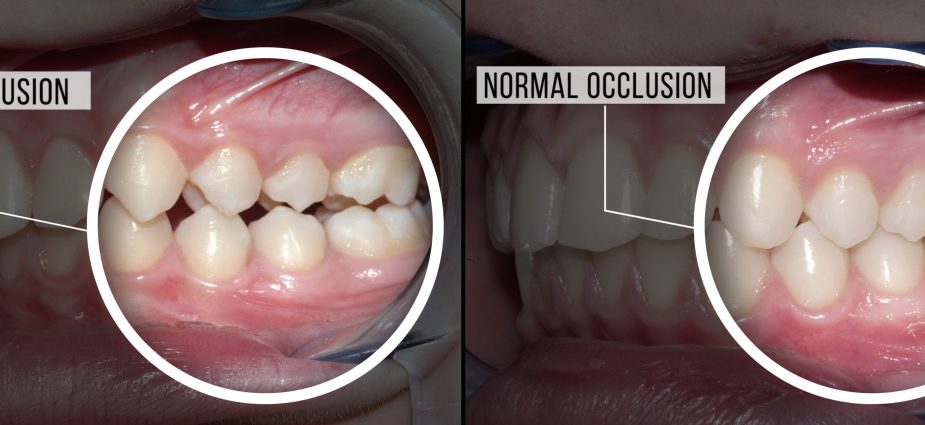
What’s Normal and What’s Not? Classes of Occlusion
Dentists consider occlusion to be normal when the upper and lower teeth fit nicely and evenly together with the least amount of destructive interferences.
A Class I occlusion is what is typically considered the “ideal” and least destructive occlusal relationship. Although this is a gross oversimplification, a Class I occlusal relationship is often identified by the lower anterior incisors sitting just behind the upper anterior incisors when biting down. Malocclusion is defined as improper occlusion, or the abnormal coming together of the teeth.
A Class II malocclusion is identified by the lower anterior incisors positioned significantly behind the upper anterior incisors when biting down. Commonly referred to as an overbite, it is typical of a Class II malocclusion to find the lower front teeth hitting close to or on the gum tissue behind the upper teeth. If left untreated, a Class II malocclusion can result in discomfort, excessive wear of the front teeth, bone damage and the eventual loss of the upper anterior incisors.
A Class III malocclusion is identified by the lower anterior incisors positioned edge to edge with, or just in front of, the upper anterior incisors. This type of malocclusion may also be referred to as a crossbite.
It is important to note that just because teeth might not look “normal” or fall into the classification of proper occlusion, if there is an absence of signs or symptoms of pathology, then occlusion is most likely “normal” for that individual. Likewise, it is possible for a person with a “normal” occlusion to experience pain and dental problems and possibly require occlusal adjustments.
How Malocclusion Can Affect Your Oral Health
There are five main muscles that control your ability to open and close your mouth. Together these muscles can generate tremendous forces when chewing, clenching and grinding your teeth. If a misalignment of the teeth is present, these large forces can be translated form the misaligned teeth as destructive forces to the ligaments and bone that hold the teeth in place, the muscles of the head and neck and the jaw joint.
If left untreated, malocclusion could lead to:
- Chronic headaches
- Temporomandibular joint disorder (TMJ)
- Muscle pain
- Tooth movement
- Tooth loss
- Injuries to the teeth
- Tooth wear
- Tooth sensitivity
If you and your dentist determine that your occlusion is contributing to and/or causing dental problems – whether pain, chipped or broken teeth, failing restorations or other consequences of a bad bite – a treatment plan may be developed to adjust your occlusion. In order to do this, your dentist will require a full series of intraoral radiographs (X-rays), photographs and impressions of your teeth so that models can be made of how they come together. Your dentist may also want a CT of your tempromandibular joint (TMJ).
Using these materials as a basis for further study, your dentist will determine the best way to modify your teeth to improve your occlusion. This may involve reshaping, restoring (dental crowns, dental veneers, composite bonding), or repositioning (orthodontics) some or all of your teeth. In severe circumstances, surgery to reposition the jaw – called orthognathic surgery – may be required.
Occlusion & Cosmetic Dentistry
When you visit the dentist for a single filling or crown, chances are that he or she won’t need to change or adjust your overall occlusion, as long as you haven’t had any symptoms of malocclusion up to that point. Rather, your dentist will likely just conform to or manage your current occlusion, keeping it relatively the same as it was before the restoration was fitted.
However, if your dentist identifies problems such as wear, tooth mobility, muscle pain or other signs of malocclusion, then your bite may need to be adjusted.
If you are interested in more comprehensive cosmetic dental treatment, ensuring a stable bite becomes even more important to your oral health and the long-term durability and functionality of the dental veneers or crowns your dentist places. A stable occlusion is a requirement for long-lasting and beautiful cosmetic dentistry. If your occlusion is not properly managed during the planning and treatment phases, your cosmetic dentistry could be at risk for early failure.
Ways of Thinking About Occlusion
Essentially, dentists approach occlusion in five different ways. Each of these theories about occlusion has merit, and treatments based on each have been successful. The theory your dentist chooses to follow can depend upon a number of factors. These factors may include patient characteristics and type of overall treatment that is being planned, as well as your dentist’s education, training and various other considerations.
- Intercuspal theory: The occlusion or bite is determined by tooth contact.
- Musculoskeletal/centric relation theory: The occlusion or bite is determined by the balance of the jaw muscles and not by how the teeth come together.
- Neuromuscular theory: The occlusion or bite is determined by gravity and based on where the jaw muscles are most relaxed.
- Most posterior retruded position theory: The occlusion or bite is determined by how the ligaments brace the components of the jaw joint, particularly toward the rearmost hinge axis.
- Anterior protrusive position theory: The occlusion or bite is determined by how the muscles brace the components of the jaw joint.
These theories of how a person’s teeth can come together have several aspects in common. First, they share the idea that the upper and lower teeth should fit together evenly, with no one tooth hitting higher than another. Also, when the upper and lower jaws move from side to side, the front teeth should touch and the back teeth should not. What differs among these theories is where the jaw or temporomandibular joint should be positioned during treatment.


