Teeth Whitening: How it Works and What it Costs
Medically Reviewed by: Larry Addleson, DDS, FAACD

On this page: Teeth whitening options | Shade guides | Whitening risks | Cost of whitening | En Español
Teeth whitening is one of the most popular cosmetic dentistry treatments offering a quick, non-invasive and affordable way to enhance a smile. Universally valued by men and women alike, whitening (or bleaching) treatments are available to satisfy every budget, time frame and temperament. Whether in the form of professionally administered one-hour whitening sessions at a dental office or cosmetic spa, or home-use bleaching kits purchased at your local drugstore, solutions abound.
Virtually everyone who opts for a teeth whitening solution sees moderate to substantial improvement in the brightness and whiteness of their smile. That said, it’s not a permanent solution to discoloration and requires maintenance or “touch-ups” for a prolonged effect.
In this article we break down everything related to teeth whitening, including the process of tooth discoloration, what causes staining, the various treatment options available, and their associated risks and costs.
Bleaching vs. Whitening: What’s the Difference?
According to the FDA, the term “bleaching” is permitted to be used only when the teeth can be whitened beyond their natural color. This applies strictly to products that contain bleach — typically hydrogen peroxide or carbamide peroxide.
The term “whitening” on the other hand, refers to restoring a tooth’s surface color by removing dirt and debris. So technically speaking, any product that is used to clean the teeth (like a toothpaste) is considered a whitener. Of course, the term whitening sounds better than bleaching, so it is more frequently used — even when describing products that contain bleach.
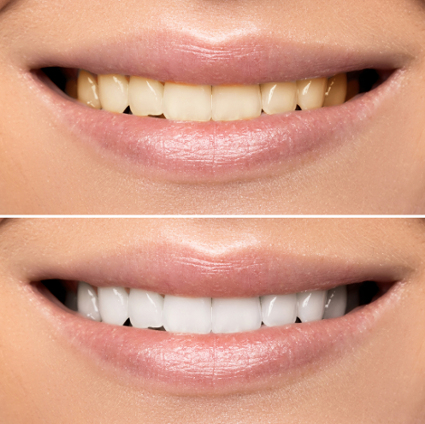
The bleach preference for in-office whitening, where time is limited, is powerful and fast-acting hydrogen peroxide. When used in bleaching teeth, hydrogen peroxide concentrations range from approximately nine percent to 40 percent.
By contrast, the bleach of preference for at-home teeth whitening is slower-acting carbamide peroxide, which breaks down into hydrogen peroxide. Carbamide peroxide has about a third of the strength of hydrogen peroxide. This means that a 15 percent solution of carbamide peroxide is the rough equivalent of a five percent solution of hydrogen peroxide.
An Examination of Tooth Enamel
Most of us start out with sparkling white teeth, thanks to their porcelain-like enamel surface. Composed of microscopic crystalline rods, tooth enamel is designed to protect the teeth from the effects of chewing, gnashing, trauma and acid attacks caused by sugar. But over the years enamel is worn down, becoming more transparent and permitting the yellow color of dentin — the tooth’s core material — to show through.
During routine chewing, dentin remains intact while millions of micro-cracks occur in the enamel. It is these cracks, as well as the spaces between the crystalline enamel rods, that gradually fill up with stains and debris. As a result, the teeth eventually develop a dull, lackluster appearance.
Teeth whitening removes the stains and debris, leaving the enamel cracks open and exposed. Some of the cracks are quickly re-mineralized by saliva, while others are filled up again with organic debris.
Tooth Discoloration: Extrinsic vs. Intrinsic Staining
There are two categories of staining as it relates to the teeth: extrinsic and intrinsic.
Extrinsic stains are those that appear on the surface of the teeth as a result of exposure to dark-colored beverages, foods and tobacco, and routine wear and tear. Superficial extrinsic stains are minor and can be removed with brushing and prophylactic dental cleaning. Stubborn extrinsic stains can be removed with more involved efforts, like teeth whitening. Persistent extrinsic stains can penetrate into the dentin and become ingrained if they are not dealt with early.
Intrinsic stains are those that form on the interior of teeth. Intrinsic stains result from trauma, aging, exposure to minerals (like tetracycline) during tooth formation and/or excessive ingestion of fluoride. In the past, it was thought that intrinsic stains were too resistant to be corrected by bleaching. Today, cosmetic dentistry experts believe that even deep-set intrinsic stains can be removed with supervised take-home teeth whitening that is maintained over a matter of months or even a year. If all else fails, there are alternative cosmetic solutions to treat intrinsic staining, such as dental veneers.
Teeth Whitening vs Dental Veneers
Whitening and veneers are two popular smile makeover treatment options. Weigh their pros and cons with your needs.
What Causes Tooth Staining?
Age: There is a direct correlation between tooth color and age. Over the years, teeth darken as a result of wear and tear and stain accumulation. Teenagers will likely experience immediate, dramatic results from whitening. In the twenties, as the teeth begin to show a yellow cast, whitening may require a little more effort. By the forties, the yellow gives way to brown and more maintenance may be called for. By the fifties, the teeth have absorbed a host of stubborn stains which can prove difficult (but not impossible) to remove.
Starting color: We are all equipped with an inborn tooth color that ranges from yellow-brownish to greenish-grey, and intensifies over time. Yellow-brown is generally more responsive to bleaching than green-grey.
Translucency and thinness: These are also genetic traits that become more pronounced with age. While all teeth show some translucency, those that are opaque and thick have an advantage: they appear lighter in color, show more sparkle and are responsive to bleaching. Teeth that are thinner and more transparent – most notably the front teeth – have less of the pigment that is necessary for bleaching. According to cosmetic dentists, transparency is the only condition that cannot be corrected by any form of teeth whitening.
Eating habits: The habitual consumption of red wine, coffee, tea, cola, carrots, oranges and other deeply-colored beverages and foods causes considerable staining over the years. In addition, acidic foods such as citrus fruits and vinegar contribute to enamel erosion. As a result, the surface becomes more transparent and more of the yellow-colored dentin shows through.
Smoking habits: Nicotine leaves brownish deposits which slowly soak into the tooth structure and cause intrinsic discoloration.
Drugs / chemicals: Tetracycline usage during tooth formation produces dark grey or brown ribbon stains which are very difficult to remove. Excessive consumption of fluoride causes fluorosis (discoloration marked by the appearance of faint white marks on the teeth) and associated areas of white mottling.
Grinding: Most frequently caused by stress, teeth grinding (gnashing, bruxing, etc.) can add to micro-cracking in the teeth and can cause the biting edges to darken.
Trauma: Falls and other injuries can produce sizable cracks in the teeth, which collect large amounts of stains and debris.
What are Your Whitening Options?
Three major teeth whitening options are available today. All three rely on varying concentrations of peroxide and varying application times.
In-Office Whitening
Significant color change in a short period of time is the major benefit of in-office whitening. This protocol involves the carefully controlled use of a relatively high-concentration peroxide gel, applied to the teeth by the dentist or trained technician after the gums have been protected with a paint-on rubber dam. Generally, the peroxide remains on the teeth for several 15 to 20 minute intervals that add up to an hour (at most). Those with particularly stubborn staining may be advised to return for one or more additional bleaching sessions, or may be asked to continue with a home-use system.
Cost: $650 per visit (on average) nationwide.
(Read more about in-office whitening)
Professionally Dispensed Take-Home Kits
Many dentists are of the opinion that professionally dispensed take-home whitening kits can produce the best results over the long haul. Take-home kits incorporate an easy-to-use lower-concentration peroxide gel that remains on the teeth for an hour or longer (sometimes overnight). The lower the peroxide percentage, the longer it may safely remain on the teeth. The gel is applied to the teeth using custom-made bleaching trays that resemble mouth guards.
Cost: $100 to $400.
(Read more about take-home whitening)
Over-the-Counter Products
The cheapest and most convenient of the teeth whitening options, over-the-counter bleaching involves the use of a store-bought whitening kit, featuring a bleaching gel with a concentration lower than that of the professionally dispensed take-home whiteners. The gel is applied to the teeth via one-size-fits-all trays, strips or paint-on applicators. In many cases this may only whiten a few of the front teeth unlike custom trays that can whiten the entire smile.
Cost: $20 to $100.
How White Can You Go? A Matter of Esthetics
Results are subjective, varying considerably from person to person. Many are immediately delighted with their outcome, while others may be disappointed. Before you embark on any whitening treatment, ask your dentist for a realistic idea of the results you are likely to achieve and how long it should take to achieve them.
Shade Guides
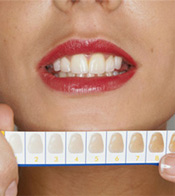
In the dental office, before-and-after tooth color is typically measured with shade guides. These are hand-held displays of wide ranges of tooth colors. (Dentists also use them in choosing crown and other restoration shades.)
The standard-setter among them has long been the Vitapan Classic Shade Guide. This shade guide standard incorporates 16 shades, systematically arranged from light to dark into four color groups, and provides a universal tooth-color terminology.
While whitening can occasionally lighten tooth color by nine or more shades, most of those who bleach their teeth are likely to see a change of two to seven shades.
Risks
Teeth whitening treatments are considered to be safe when procedures are followed as directed. However, there are certain risks associated with bleaching that you should be aware of:
- Sensitivity: Bleaching can cause a temporary increase in sensitivity to temperature, pressure and touch. This is likeliest to occur during in-office whitening, where higher-concentration bleach is used. Some individuals experience spontaneous shooting pains (“zingers”) down the middle of their front teeth. Individuals at greatest risk for whitening sensitivity are those with gum recession, significant cracks in their teeth or leakage resulting from faulty restorations. It has also been reported that redheads, including those with no other risk factors, are at particular risk for tooth sensitivity and zingers. Whitening sensitivity lasts no longer than a day or two, but in some cases may persist up to a month. Some dentists recommend a toothpaste containing potassium nitrate for sensitive teeth.
- Gum irritation: Over half of those who use peroxide whiteners experience some degree of gum irritation resulting from the bleach concentration or from contact with the trays. Such irritation typically lasts up to several days, dissipating after bleaching has stopped or the peroxide concentration lowered.
- Technicolor teeth: Restorations such as bonding, dental crowns or veneers are not affected by bleach and therefore maintain their default color while the surrounding teeth are whitened. This results in what is frequently called “technicolor teeth.”
Maintaining Your Results
To extend the longevity of newly whitened teeth, dentists are likely to recommend:
- At-home follow-up or maintenance whitening – implemented immediately or performed as infrequently as once a year.
- Avoiding dark-colored foods and beverages for at least a week after whitening.
- Whenever possible, sipping dark-colored beverages with a straw.
- Practicing excellent oral hygiene – brushing and flossing after meals and at bedtime.
Caveats
In addition to the aforementioned risk factors, a number of caveats should be considered before undergoing teeth whitening:
- No amount of bleaching will yield “unnaturally” white teeth.
- Whitening results are not fully seen until approximately two weeks after bleaching. This is an important consideration if you are about to have ceramic restorations and want to be sure the color matches that of your newly bleached teeth.
- If cosmetic bonding, porcelain veneers or other restorations are part of your treatment plan, they should not be placed until a minimum of two weeks following bleaching to ensure proper adhesive bonding, function and shade matching.
- To avoid the technicolor effect, tooth-colored restorations will likely need replacement after bleaching.
- Recessed gums often reveal their yellowish root surfaces at the gum line. That yellow color has proven difficult to bleach.
- Pregnant or nursing women are advised to avoid teeth whitening. The potential impact of swallowed bleach on the fetus or baby is not yet known.
How Much Does Teeth Whitening Cost?
The cost of teeth whitening can vary quite significantly from product to product, procedure to procedure.
Professional, in-office teeth whitening is the most expensive option with a national average of $650 per visit (pricing can vary between $500 to $1,000). However it does have the benefit of being performed by an experienced dental professional, helping to ensure that you get the sort of results you’re looking for.
At the other end of the cost spectrum are over-the-counter strips and trays that you can buy at your local pharmacy or grocery store. These products can range from $20 to $100, making them an attractive option for those looking for a bit of smile enhancement without the higher cost of professionally administered whitening. However, it’s important to keep in mind that results can vary drastically when using these cheaper, low-concentration peroxide whiteners.
If you’re looking for a middle-ground between professional whitening and over-the-counter products, you might be a good candidate for professionally dispensed take-home kits. Prescribed by a dentist, these kits range in cost from $100 to $400, and can potentially deliver results similar to those you’d get in-office at the hands of a dentist.
Keep in mind that whitening results are not permanent, meaning that if you want to maintain your whitened smile, you’ll need to continue getting treatments as the effects wane.
[updated April 18, 2019]
About the Reviewer

Lawrence Addleson, DDS, FAACD, of San Diego, CA is an internationally recognized leader in the field of aesthetic cosmetic dentistry. In 1993 he earned his accreditation with the American Academy of Cosmetic Dentistry (AACD) and is one of the few dentists worldwide to complete the rigorous criteria for both accreditation and fellowship, the most prestigious level of clinical excellence achievable within the AACD. Dr. Addleson has held many top positions within the AACD, including president, member of the Board of Directors, and twice chairman of the Board of Governors.
Dr. Addleson earned his DDS in 1969 from the University of Southern California School of Dentistry, and is the founder of The Art of Dentistry, a premier cosmetic and restorative dentistry practice located in San Diego.