Oral Thrush Causes, Symptoms and Treatment
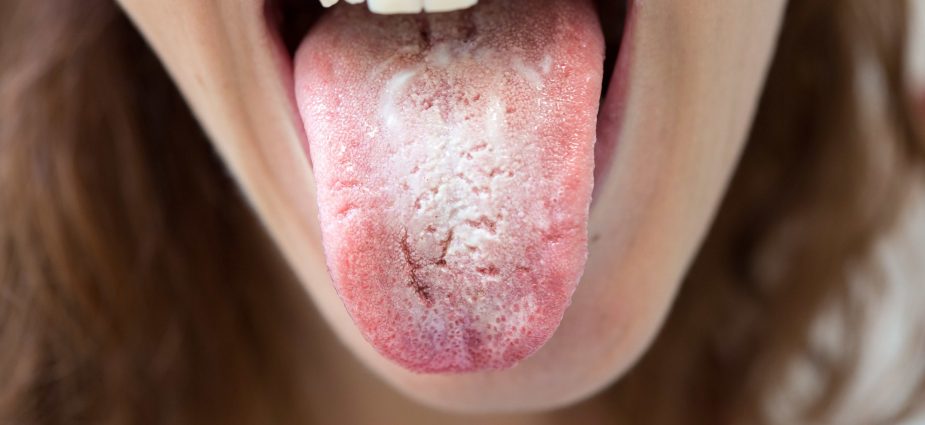
Oral thrush – or oral pseudomembranous candidiasis – is a fungal infection of the mouth common among denture wearers, infants and people with weakened immune systems. The most common human fungal infection, thrush presents as slightly raised removable plaques (resembling cottage cheese) on the tongue or inner cheek. It can also affect the roof of the mouth, gums, tonsils or back of the throat.
There are three other forms of oral candidiasis infections:
- Erythematous candidiasis appears as red patches on the roof of the mouth and tongue.
- Hyperplastic (chronic) candidiasis resembles the more common type, but cannot be scraped off.
- Angular cheilitis looks like red sores that develop in the corners of the mouth.
Causes
Oral thrush is caused primarily when there is an overgrowth of Candida albicans, a yeast normally present in the mouth in small quantities and kept in balance by helpful bacteria in the body. Less frequently, ith may also be caused by an overgrowth/infection of the Candida glabrata or Candida tropicalis yeasts, which also are present in the mouth.
Dry mouth, high blood and salivary sugar levels (diabetes), and prolonged use of certain antibiotics or corticosteroid therapy (asthma inhalers) can upset the body’s natural balance of friendly bacteria that would otherwise fight off a yeast infection. This allows overgrowth of Candida and leads to thrush.
Symptoms
There are several symptoms associated with the development of the fungal infection. In addition to having a white, yellow or cream-colored curd-like appearance, oral thrush can cause a burning sensation in the mouth, soreness and/or sensitivity to acidic and spicy foods, an unpleasant taste in the mouth and bad breath (halitosis). Scraping the white lesions from the soft tissues (mucosa) of the mouth may cause bleeding and a painful sensation, revealing red and inflamed surfaces underneath.
Candidal infections can lead to a diaper rash in infants that does not heal with the use of ointments (yeast passes through the baby’s stool), in addition to a rash in the infant’s mouth. Mothers and their infected infants can pass thrush back and forth. For a breastfeeding mother, Candidal infection could result in burning, painful nipples. Candidal infections can also cause vaginal yeast infections in women.
Candidiasis is not limited to the mouth and, if left untreated, can spread to other parts of the body (throat, vagina, skin). Although rare, oral thrush can spread to other organs of the body, but this is usually limited to immunocompromised individuals.
Your dentist can diagnose it by examining your mouth and brushing the lesions away. If necessary, microscopic testing can be used for confirmation.
Considerations and Risk Factors
A number of factors can put an individual at higher risk for an oral thrush or candidiasis infection. Women who are pregnant, women taking birth control pills and those who experience persistent dry mouth (caused by systemic conditions or medications such as antidepressants) are more likely to develop a candidal infection. Other at-risk individuals include:
Newborns/Nursing Mothers: Babies and nursing mothers must both be properly treated to prevent passing the Candidal infection back and forth. Dentists or healthcare providers can prescribe mild antifungal medications to treat oral infections, and an antifungal cream may be needed for treating the breasts.
Diabetics: Individuals with diabetes have a reduced resistance to infection, so they may experience an increased incidence of oral thrush. To prevent oral infections, dentists may recommend medicated mouth rinses or more frequent dental hygiene appointments.
People with Asthma/Chronic Obstructive Pulmonary Disease (COPD): The use of inhaled corticosteroids has been shown to increase an individual’s risk for oral thrush. This risk can be reduced by using a spacer and rinsing the mouth after using the inhaler.
Denture Wearers: A common contributor to oral thrush is denture stomatisis, which occurs when the gums and soft tissue of the mouth are irritated and inflamed from wearing a denture that doesn’t fit well or hasn’t been properly cleaned on a regular basis. This condition creates an environment that is ideal for Candida growth.
Smokers: The use of tobacco has been identified as a contributing factor in oral thrush infection.
Immune deficiencies (HIV, Chemotherapy/Cancer Patients): Deficiencies in the immune system that result from chemotherapy, radiation treatments or HIV infection can dramatically change the balance of the protective mechanisms in the body that would otherwise fight off an oral thrush infection. An individual’s ability to fight infection determines the severity of oral thrush and the fungal infection overall. Individuals with HIV are prone to severe forms of thrush in their mouth or esophagus, as well as spread of the infection to the intestines. Prolonged antifungal treatment may be necessary for individuals with severe infections and/or those who are immunocompromised.
Treatments
Oral thrush treatment starts with the management of the conditions that caused development of the fungal infection. For example, if you have developed it as a result of using a particular antibiotic, you should speak with your physician immediately about getting an alternative medication.
If you wear dentures, they should be removed from the mouth at bedtime and thoroughly cleaned. An antimicrobial mouth rinse may also be recommended by your dentist for use as a denture disinfecting agent.
If you are diabetic, you must carefully monitor and control your blood glucose levels. Those who are immunocompromised may need oral or IV antifungal medications to control the Candidal infection on an ongoing basis.
Practicing good oral hygiene is also important, as well as limiting the amount of sugary and yeast-containing foods that you eat.
Mild cases may be managed without medications. Drinking acidic liquids such as orange juice and eating yogurt can help to rebalance the natural bacteria that keep the Candida yeast in check.
Your dentist will develop a treatment plan for you based on your specific condition and the nature of your oral thrush infection. Medications include antifungal mouth rinses, lozenges, creams and oral tablets. In some cases, a combination of oral tablets and lozenges are used to treat severe infections. As many as 14 days of treatment with antifungal medications may be necessary to treat severe infections.
In some instances, generic brands of the medications are available, which will help to lessen the cost of any treatment regimen prescribed for you by your dentist. Dental insurance will cover the cost of prescription medications to treat oral thrush, and some medications are available over-the-counter.
Topical medications used to treat thrush include nystatin (creams, ointments, powder and oral solution) or clotrimazole lozenges. Nystatin powder or ointments may be applied to the affected mucosa and/or inside the thoroughly cleaned dentures and worn. Nystatin solution is used to rinse the mouth. It is safe to swallow for treatment of candidiasis affecting the throat.
Oral tablets of fluconazole may also be used (with an estimated wholesale price of $104.00 for treatment). Other antifungal medications are also available and may be prescribed by your dentist depending upon your condition and diagnosis.![]()


