Oral Herpes
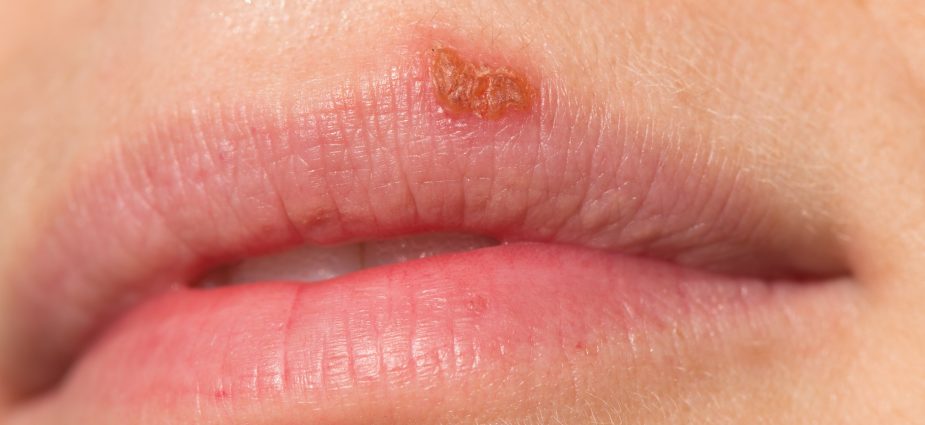
Widely known as cold sores or fever blisters, herpes labialis is a common and generally benign viral condition that produces painful and frequently unsightly sores on the lips or adjacent skin. The virus may also cause sores on the bone-bearing tissues such as the gums and the roof of the mouth.
In the U.S., up to 60 percent of children are exposed to the virus by late puberty and nearly 90 percent of adults carry the virus by age sixty. Only about 40 percent of those infected experience outbreaks of oral herpes.
If you are in relatively good health, oral herpes is a self-limiting annoyance. Even left untreated, it runs its course in about seven to 14 days. And while it may affect merely the quality of life in those who are otherwise healthy, the condition can be dangerous among infants, the elderly and those who are immunocompromised by conditions such as HIV/AIDS, leukemia or organ transplantation.
Causes
Dentists and medical professionals refer to the causative virus as herpes simplex type 1, which is one among more than 80 known herpes viruses. Although far less dangerous than other herpes viruses, herpes simplex type 1 shares an important similarity with them: Once the infection enters the body, it persists for life, frequently in a latent form.
The infection spreads to others by oral contact. In the presence of active sores, the virus is likely to be shed into saliva. So it is important to avoid oral contact. This means:
- No kissing or other forms of skin contact with people.
- No sharing of food, drink or dining and kitchen implements.
- No sharing of dental implements such as toothbrushes and dental floss.
- No sharing of towels.
- Individuals with an active herpetic sore or those who are recovering from an outbreak should avoid close contact with infants and those who are immunosuppressed.
Triggers
Certain conditions can trigger an outbreak of cold sores. They include:
- Stress – whether emotional or physical
- Pain
- Surgery
- Fever
- Irritants such as exposure to sun, wind and cold
- Lack of sleep
- Menstruation
- Immunosuppression
What to expect
After the initial infection, the virus travels along the trigeminal nerve (with several branches in the upper and lower face) to a collection of nerve cells in the brain known as trigeminal ganglion, where it remains dormant until reactivation. Once activated, the virus travels down the nerve and leads to the development of a cold sore or series of lesions at the site of initial entry inside the mouth.
Development and healing of these sores goes through six stages over the course of seven to 14 days:
- The prodrome, where there is a prickling, tingling or itching sensation, but no visible sore.
- Swelling, slight redness and pain. Eating and drinking become difficult.
- The eruption of a blister or cluster of blisters.
- The breakdown of the blisters into shallow, yellowish ulcers.
- The emergence of a hard, irregular crust, with cracking and some bleeding.
- The condition recedes to a residue of slight swelling and redness and heals without scarring.
Seeking Professional Care
There is general agreement in both the medical and dental communities that compared to medical doctors, dentists are more likely to encounter patients with oral herpes, and thus are better able to diagnose the condition.
Also, since they may develop following routine dental procedures, dentists are in a position to offset the condition by prescribing preventive medications such as creams or pills before proceeding with treatment. These drugs are started 24 hours before dental treatment and continued for two days afterwards.
Diagnosis: When and if to Biopsy
Diagnosis of oral herpes is straightforward and frequently based on visible signs or reported symptoms. However, when the patient is compromised or diagnosis is in question, a diagnostic smear or biopsy may be performed for confirmation.
Intraoral Herpes or Canker Sores?
Intraoral herpes may be confused with canker sores. Both conditions have small, painful lesions that resolve on their own in seven to 14 days. But there are notable differences:
- Intraoral herpes affects bone-bearing tissues of the roof of the mouth and the gums, while canker sores appear on soft, movable tissue – on the insides of the lips or cheek and the back of the throat.
- Herpes sores start off as little bumps which break apart and leave small ulcers. Canker sores are sores from the outset.
- Canker sores are larger than herpes sores and are slower to heal.
- Herpes sores tend to reappear in the same place, while canker sores occur in different areas within the mouth.
Treatments
Topical application of ice, alcohol or lip balms may relieve the symptoms of cold sores.
A cold sore outbreak may be pre-empted or aborted by application of Peniclovir (Denavir), an antiviral prescription cream, or Docosanol (Abreva), an over-the-counter cream, early during the onset of symptoms. Both are easy to apply. (Note: Patients must be sure to wash their hands after applying these or any topical herpes medication.)
Oral antiviral medications are typically reserved for those who have frequent or severe outbreaks of cold sores and those who are immunocompromised. For maximal efficacy, these medications also should be started during the prodrome, or within 24 hours of an outbreak.
Topical anesthetics such as lidocaine or agents such as Kaopectate that coat the gums and roof of the mouth may be used to treat the symptoms of intraoral herpes. Pain-relieving medications such as acetaminophen (Tylenol), aspirin or ibuprofen (Advil, Motrin, etc.) are also helpful. Frequent, severe recurrences may benefit from prescription oral antivirals.
An Oral Cancer Connection?
While the human papillomavirus and a couple strains of herpes virus are now regarded as possible contributors to certain types of oral cancer, we have no clear evidence that oral herpes has a causal connection to oral cancer.![]()


